The Criterions EHR adopted ICD-10 in 2012. The EHR stores ICD-10 coding with ICD-9 entries after every visit. Once ICD-10 goes into effect, planned for Oct 1, 2014, Criterions products will automatically send the ICD10 with the EDI claims.
EHR clients will have the capabilities of auto-mapping the ICD-9 to ICD-10 codes, with an exception list that can be manually resolved by the users.
TCMS clients, without the comprehensive and integrated Criterions EHR, will be able to manually enter the ICD-10 in the Diagnosis setup. Users will manually find the corresponding ICD-10 codes and put them in the setup.
For more information on ICD-10, please click on the following links:
(Clicking on any of these links will open the link in a new window)
CMS/Medicare ICD-10 Coding FAQ's
AMA Transaction Code Set Standards for ICD10-codes
AHIMA ICD-10
Monday, December 31, 2012
Friday, December 21, 2012
TCMS Version 4.8.3 – What’s New, What’s Fixed, etc
( any image can be enlarged by clicking on it)
This version includes version 4.8.2 – please update to 4.8.3
Procedure Code Financial Analysis report adjustment
When generating a Procedure Code Financial Analysis report, specifically by Insurance Types and including patient names, the report was not including services generated for now-inactive carriers... causing a noted difference between the detailed and the summarized versions of the report. This has now been corrected by including the services in the detailed report.
When generating a Procedure Code Financial Analysis report, specifically by Insurance Types and including patient names, the report was not including services generated for now-inactive carriers... causing a noted difference between the detailed and the summarized versions of the report. This has now been corrected by including the services in the detailed report.
Document edits now display in preview immediately after saving
When editing a patient's document, the changes will now display in the preview portion of the screen immediately after saving (no longer need to refresh the screen).
Tickler System capacity increased
The Tickler System text box character capacity is now increased to accommodate up to 500 characters.
Worker’s Compensation form adjustment
The Worker’s Compensation form "C4.3" will now allow for the simultaneous selections of progress note fields 2A (scheduled loses) and 2B (non-scheduled losses).
A new field for Medicare Secondary Payor (MSP) Type identifier is now available
For claims billed electronically, the MSP insurance type code (submitted in loop 2000B within the SBR 05 segment) identifies the type of other insurance that is the basis for the beneficiary’s MSP status.
TCMS now has a new custom field named "Reason why Medicare is secondary" in the Patient Custom Field feature, located in the patient's Demographics screen. The electronic claim file builds the Medicare secondary insurance type code based on the custom field value entered here.
Here is a list of the MSP Provisions as provided by Medicare:
Correction made posting electronic United Healthcare secondary payments
United Healthcare secondary payments were sporadically posting as either GHI payments or as primary payments. This is now corrected and they will now post appropriately.
Workflow Queue is now freeze-free
The Workflow queue was sometimes "freezing" in some situations after printing a document. This problem is now addressed and this feature will no longer freeze for the affected clients.
TCMS is now Press Ganey patient-survey-friendly
A CSV-file export of patient data can now be generated from the Scheduling module for submission to Press Ganey and for the purposes of client-specific patient surveys. Press Ganey collects the data and randomly determines which of the patients are surveyed. The use of this feature requires activation by Criterions. Once activated, a Press Ganey Format option appears in the export feature:
A new ESB Queue User Right is available
There is now a new User Right which allows for the removal of entries from the Electronic Superbill(ESB) Queue feature. Prior to this version, any user with rights to the ESB Queue had the ability to remove entries from the ESB Queue. With this update, the User Right is selected by default so that the user can continue removing entries, but the right to do so can now be managed:
Patient Balance due amount is now displayed in the Patient Search screen
While searching for a patient within the Patient Search screen, in addition to the total account balance, you can now also see the "Patient Balance." This will display the total balance due from the patient, based on all services with a balance that are due from "Self."
Three changes are now in effect within the Provider Number Setup screen
1) When using the "Copy Provider Number" feature, the "Pay To" and the "Billing Address" fields will now also be copied;2) When using the "Setup by Insurance Type" feature, the user can now also enter the "Pay To" and the "Billing Address" information;
3) While using either of these two features, no existing data will be removed.
TCMS now utilizes the latest version of PDF Creator v. 1.4.3
This version of TCMS distributes the latest PDF Creator installation files and will install them automatically while the user accesses the older version of PDF Creator.
Medicaid form adjustment made to the "Total" calculations
Under certain circumstances only, the "Total" amount field of the Medicaid form was not calculating correctly. This problem has now been addressed.
ERx import adjustment made to the incoming file's distribution
Under certain circumstances only, an eRx response was distributed to the user's desktop rather than the appropriately designated workstation's folder. This problem has now been addressed.
FaxQ now validates the required 10 byte format
A adjustment was made to the FaxQ internal table that will ensure all fax numbers are formatted to exactly 10 digits/bytes.
While generating the Procedure Code Financial Analysis report, specifically for select insurance carriers, the report was not limited to the selected carriers. This problem has now been addressed.
Under certain circumstances only, anesthesia minutes were not printing on the CMS-1500 form. This problem has now been addressed.
New User Rights "Limited Access" option is now available
In the User Right's User Setup screen for all users, there is now a new feature labeled "Limited Access" which will limit the user's access to only patients that the user is pre-selected as "authorized" to access (a feature that is available in the patient's Additional Information screen).
Ability to filter by Procedure Group added to Claims Ledger
A new filter option is now avvailable in a patient's Claims Ledger. Along with previously available claim filters by service date span, by carrier, and/or by location, the user can now also filter services by Procedure Group.
When a user (other than a physician) is using the eRx feature, a prompt is generated asking who the prescribing doctor (Master Physician) is. This prompt was not appearing in a recent version. This problem has now been addressed.
A new "Institutional" claim identifier is now available for Facilities
Facilities (in the Facility Setup screen) now have a checkbox available that, if checked, will identify all claims with that facility attached as Institutional claims and will be picked up when creating an "Institutional" EMC file.
Note that an Institutional-specific claim file must be created for such claims to be picked up... claims with an Institutional facility will not be picked up when creating an otherwise commercial EMC file.
A Documents Usage report is now available
A new report, the Document Usage report, is now available. This report offers a broad view of the Document Catagories and their total size (in MB's) and total number of Documents in each Category. The resulting report can be sorted in a number of ways, and can also be exported to an MS Excel file for further analysis.
A Documents Usage report is now available
A new report, the Document Usage report, is now available. This report offers a broad view of the Document Catagories and their total size (in MB's) and total number of Documents in each Category. The resulting report can be sorted in a number of ways, and can also be exported to an MS Excel file for further analysis.
This version also contains a few other minor bug fixes and improvements
- The Electronic Worker’s Compensation OPT/PT has been corrected to communicate with the FTP server for iHCFA.
- Confirmed appointments are included as Appointments made when generating a Scheduling Patient List.
- In the Documents module, the the "appointment" merge fields will not regard the order they appear in within the document or the existence of past or future appointments.
- The "location" name displayed at the bottom-left corner of the TCMS splash screen is expanded to accomodate the display of longer location names.
- When multiple validation reports are uploaded together to TCMS, they will be loaded individually (which actually increases speed and helps to prevent error).
- Ticklers created without user-set delays will no longer wait for default time, and will generate when TCMS is opened by the user (this helps to prevent "ghost" ticklers).
- Checkouts in the Scheduler's ESB will generate the checked-out icon.
- Schedules and Resource Monitors will now update when schedule changes occur on the individual patient's Appointments screen.
- end
Tuesday, December 18, 2012
TCMS Version 4.8.1 – What’s New, What’s Fixed, etc
(RE-POST FROM AUGUST 2012)
Collection Module error with Documents is fixed.
Some TCMS users were receiving an “EOF error” under certain conditions while printing Bulk Documents from within the Collection Module. This will no longer happen
Duplicate check number posting errors are now prevented
If two checks containing the same check number were posted, there was a possibility the funds would be drawn from the wrong check, causing a “negative” amount posted from the check.
A database trigger has now been enabled to ensure that this no longer occurs.
New notation added to the Daily Transaction report
Due to the nature of the Daily Transaction Report not showing inactive locations, or the user running the report not having user rights to a given location, we have added a notation at the bottom of the report to reflect the data that is used to generate the report.
The notation reads: “This report does not generate data from transactions performed in inactive locations.
This report will also not display data from transactions performed in locations for which that user does not have rights”.
Institutional Billing now available through TCMS’s Emdeon Claim Center
TCMS now offers Institutional Billing through the Emdeon Clearinghouse.
To accomplish this, place a checkmark on the new option in Practice Defaults Setup screen labeled “Send Institutional Claims to Emdeon”. Then, while creating the EMC file, select the “Institutional” option.
ERx files now save correctly to the intended (temp) folder
ERx files were inadvertently downloaded to the user’s desktop instead of a temp folder. This has been corrected.
A field in the Worker’s Comp HP1 for now populates appropriately
The Workers Comp HP1 form was not populating the “County” fields in all cases. This has now been corrected.
Printed HCFA/CMS-1500 forms will generate all modifiers
CPT/Claims that contained four modifiers were not generating all of the modifiers consistently.
The modifiers on the CMS-1500 form will now fill all the boxes when there are 4 modifiers for a given CPT.
Daily Transaction report with Custom Fields is now optimized
There was an issue with the Daily Transaction report in which the use of Custom Fields would cause the report to slow down. The database elements are now optimized for use with custom fields.
Workflow Queue error addressed
The Workflow Queue had an issue with the List View under some conditions in which it would not display the document, but rather generate and error,
“Archive does not exist”. This problem has now been addressed.
HCFA/CMS-1500 error addressed
Printing a HCFA/CMS-1500 was sometimes generating an error, stating “Error in Execute: 998 Failed to Retrieve Error Message from Print Engine.”
This was related to 5010 requirement changes. A database change has been put in place to ensure the error will no longer display.
(RE-POST FROM AUGUST 2012)
Collection Module error with Documents is fixed.
Some TCMS users were receiving an “EOF error” under certain conditions while printing Bulk Documents from within the Collection Module. This will no longer happen
Duplicate check number posting errors are now prevented
If two checks containing the same check number were posted, there was a possibility the funds would be drawn from the wrong check, causing a “negative” amount posted from the check.
A database trigger has now been enabled to ensure that this no longer occurs.
New notation added to the Daily Transaction report
Due to the nature of the Daily Transaction Report not showing inactive locations, or the user running the report not having user rights to a given location, we have added a notation at the bottom of the report to reflect the data that is used to generate the report.
The notation reads: “This report does not generate data from transactions performed in inactive locations.
This report will also not display data from transactions performed in locations for which that user does not have rights”.
Institutional Billing now available through TCMS’s Emdeon Claim Center
TCMS now offers Institutional Billing through the Emdeon Clearinghouse.
To accomplish this, place a checkmark on the new option in Practice Defaults Setup screen labeled “Send Institutional Claims to Emdeon”. Then, while creating the EMC file, select the “Institutional” option.
ERx files now save correctly to the intended (temp) folder
ERx files were inadvertently downloaded to the user’s desktop instead of a temp folder. This has been corrected.
A field in the Worker’s Comp HP1 for now populates appropriately
The Workers Comp HP1 form was not populating the “County” fields in all cases. This has now been corrected.
Printed HCFA/CMS-1500 forms will generate all modifiers
CPT/Claims that contained four modifiers were not generating all of the modifiers consistently.
The modifiers on the CMS-1500 form will now fill all the boxes when there are 4 modifiers for a given CPT.
Daily Transaction report with Custom Fields is now optimized
There was an issue with the Daily Transaction report in which the use of Custom Fields would cause the report to slow down. The database elements are now optimized for use with custom fields.
Workflow Queue error addressed
The Workflow Queue had an issue with the List View under some conditions in which it would not display the document, but rather generate and error,
“Archive does not exist”. This problem has now been addressed.
HCFA/CMS-1500 error addressed
Printing a HCFA/CMS-1500 was sometimes generating an error, stating “Error in Execute: 998 Failed to Retrieve Error Message from Print Engine.”
This was related to 5010 requirement changes. A database change has been put in place to ensure the error will no longer display.
Wednesday, July 11, 2012
835 (ERN) FILES FROM MEDICARE
Have you stopped receiving your 835 ERN files from Medicare? Most of our clients are not experiencing this problem.
If you stopped receiving them, you may have neglected to complete the 5010 production transition agreement. We provided instructions in January and completion was required before July 1st.
If your files have stopped coming, you need to complete the form. CLICK HERE and complete the 5010 Production Transition form online. It can take 5 to 10 business days to process the form. Once it is processed, you will receive a confirmation email from NGS. There is nothing else to set up or do once confirmed and you should start receiving your 835 ERN files thereafter.
Also note that, if you submit to multiple Medicare contractors (i.e., NGS and GHI Medicare), you will need to complete the form once for each contractor.
If you need any assistance completing the form, please feel free to call our Support Services Center at (516) 466-1942, extension 2. We can help complete the form with you.
Have you stopped receiving your 835 ERN files from Medicare? Most of our clients are not experiencing this problem.
If you stopped receiving them, you may have neglected to complete the 5010 production transition agreement. We provided instructions in January and completion was required before July 1st.
If your files have stopped coming, you need to complete the form. CLICK HERE and complete the 5010 Production Transition form online. It can take 5 to 10 business days to process the form. Once it is processed, you will receive a confirmation email from NGS. There is nothing else to set up or do once confirmed and you should start receiving your 835 ERN files thereafter.
Also note that, if you submit to multiple Medicare contractors (i.e., NGS and GHI Medicare), you will need to complete the form once for each contractor.
If you need any assistance completing the form, please feel free to call our Support Services Center at (516) 466-1942, extension 2. We can help complete the form with you.
Monday, July 9, 2012
TCMS Version 4.8.0 – What’s New, What’s Fixed, etc
Electronic Superbills are now removable from the ESB Queue
You can now remove an Electronic Superbill from the queue. There is sometimes a need to remove a claim from the ESB queue because the claim may have already been written manually, or because of a scheduling error that causes the ESB Queue to contain a duplicated claim. If needed, the claim can be removed from the ESB Queue by the user by Right-mouse clicking on the entry.
The Unit Analysis report can now be exported to a CSV/Excel file
There is now an Export feature available on the Unit Analysis Report. This will allow the user to export the data of the report to a CSV/Excel file that contains the data utilized from the database for the report. The exported file is created, by default, to your C drive and users familiar with Microsoft’s Excel software can tailor the data for more customized reporting.
Verbiage changed for an option while generating Electronic Statements
For the sake of clarity, there is a verbiage change in the Electronic Statements module’s selection screen. The second option shown will now state, “Print if (select number) statements have already been printed more that 30 days ago”. There is no change in actual functionality.
Two new fields added to the Electronic Statements EMC Setup
There are 2 changes made in the Setup -> EMC section for the Statements section.
- ANSI Format, where the user can mark it as “Y” if they are going to send ANSI formatted files.
- EMF login and Password fields to allow the user to enter those fields for transmitting those files.
Labeling changed in the Patient Search screen
There is a change in the labeling when searching for a patient (F10). For accuracy, the overall balance indicator’s label will now read “Account Balance” rather than Patient Balance. There is no change in actual functionality.
Time zone adjustments within Appointments properties are now in effect
Based on the settings on your workstation, the “time” utilized within the properties of appointments in the Open Scheduler will be specific to your time zone
Credit card payment processing can now span across services
When a credit card payment is accepted for processing, you can now post the payment to multiple services. To select multiple services, enter a checkmark in the selection boxes on the right-hand side of each service, then right-click over one of the services and process the payment.
To offer an example of how the payment will be posted: if you have four services and each has a balance of $100, and your total payment to be posted is $250; the first service will receive $100, the second service would receive $100, the third service will receive $50. In other words, the payment post to the services selected from the topmost service’s balance to the bottommost service until there are no more funds left to post.
Missing option is now available
A drop down box wherein the user can select between “fax” and “email” was missing on the MG 2 Worker’s Compensation form. It is now available.
Collection claims can now remain in collections when re-billed
In the past, a claim in the Collections module would automatically be removed from Collections when re-billed to a different carrier. The user is now given the option to keep a service in Collections after rebilling the claim to another carrier in the patient’s ledger.
Worker’s Compensation MG1 form now has a “comment” field available
There is a new comment field available for the MG1 form for Worker’s Compensation.
You can now process credit card payments within the Scheduler
There is a new option available while applying a patient’s copay from their appointment in the Scheduler. TCMS has added the ability to Process Credit Card directly from the scheduler
Worker’s comp has a new field available for the HP1 form
There is a new field on the Worker’s Compensation screen to include the name of the physician that rendered the first treatment. The selections available are sourced from the practice's Referring Doctor entries. This physician’s name will appear in the second page of the HP1 form.
Improvement in denoting an overbooked appointment
The Overbook check mark in the properties of an appointment that was overbooked was sometimes inaccurately reflected due to an internal flaw. The internal logic was re-written to ensure accuracy.
Printing error fixed
In previous version of TCMS, an error while printing LABS from the Workflow queue could occur under certain conditions. An internal trigger is now added to ensure against this error.
Electronic Superbills are now removable from the ESB Queue
You can now remove an Electronic Superbill from the queue. There is sometimes a need to remove a claim from the ESB queue because the claim may have already been written manually, or because of a scheduling error that causes the ESB Queue to contain a duplicated claim. If needed, the claim can be removed from the ESB Queue by the user by Right-mouse clicking on the entry.
The Unit Analysis report can now be exported to a CSV/Excel file
There is now an Export feature available on the Unit Analysis Report. This will allow the user to export the data of the report to a CSV/Excel file that contains the data utilized from the database for the report. The exported file is created, by default, to your C drive and users familiar with Microsoft’s Excel software can tailor the data for more customized reporting.
Verbiage changed for an option while generating Electronic Statements
For the sake of clarity, there is a verbiage change in the Electronic Statements module’s selection screen. The second option shown will now state, “Print if (select number) statements have already been printed more that 30 days ago”. There is no change in actual functionality.
Two new fields added to the Electronic Statements EMC Setup
There are 2 changes made in the Setup -> EMC section for the Statements section.
- ANSI Format, where the user can mark it as “Y” if they are going to send ANSI formatted files.
- EMF login and Password fields to allow the user to enter those fields for transmitting those files.
Labeling changed in the Patient Search screen
There is a change in the labeling when searching for a patient (F10). For accuracy, the overall balance indicator’s label will now read “Account Balance” rather than Patient Balance. There is no change in actual functionality.
Time zone adjustments within Appointments properties are now in effect
Based on the settings on your workstation, the “time” utilized within the properties of appointments in the Open Scheduler will be specific to your time zone
Credit card payment processing can now span across services
When a credit card payment is accepted for processing, you can now post the payment to multiple services. To select multiple services, enter a checkmark in the selection boxes on the right-hand side of each service, then right-click over one of the services and process the payment.
To offer an example of how the payment will be posted: if you have four services and each has a balance of $100, and your total payment to be posted is $250; the first service will receive $100, the second service would receive $100, the third service will receive $50. In other words, the payment post to the services selected from the topmost service’s balance to the bottommost service until there are no more funds left to post.
Missing option is now available
A drop down box wherein the user can select between “fax” and “email” was missing on the MG 2 Worker’s Compensation form. It is now available.
Collection claims can now remain in collections when re-billed
In the past, a claim in the Collections module would automatically be removed from Collections when re-billed to a different carrier. The user is now given the option to keep a service in Collections after rebilling the claim to another carrier in the patient’s ledger.
Worker’s Compensation MG1 form now has a “comment” field available
There is a new comment field available for the MG1 form for Worker’s Compensation.
You can now process credit card payments within the Scheduler
There is a new option available while applying a patient’s copay from their appointment in the Scheduler. TCMS has added the ability to Process Credit Card directly from the scheduler
Worker’s comp has a new field available for the HP1 form
There is a new field on the Worker’s Compensation screen to include the name of the physician that rendered the first treatment. The selections available are sourced from the practice's Referring Doctor entries. This physician’s name will appear in the second page of the HP1 form.
Improvement in denoting an overbooked appointment
The Overbook check mark in the properties of an appointment that was overbooked was sometimes inaccurately reflected due to an internal flaw. The internal logic was re-written to ensure accuracy.
Printing error fixed
In previous version of TCMS, an error while printing LABS from the Workflow queue could occur under certain conditions. An internal trigger is now added to ensure against this error.
Tuesday, May 22, 2012
ASP clients can now improve connectivity
Please make sure your TCMS is on version 4.7.8 or 4.7.9 to improve connectivity to the Cloud.
Look for your current version while logging onto TCMS, or you may go to the "help" menu and select "about" . If you need assistance updating, please file an "eTrack" or call our Support Services team for assistance.
Look for your current version while logging onto TCMS, or you may go to the "help" menu and select "about" . If you need assistance updating, please file an "eTrack" or call our Support Services team for assistance.
Wednesday, May 9, 2012
TCMS Version 4.7.9 – What’s New, What’s Fixed, etc
 |
| Click Image to Enlarge |
About TCMS-to-Go
When used, it extracts a complete dataset (excluding claim or financials) for each patient within the selection criteria. This extraction includes:
• All scheduled appointments within the selected date span
• Complete Demographics
• Insurance and scanned cards
• All stored documents
• Current Medications that were prescribed within TCMS eRx
Patient’s data can then be reviewed without a connection to a live system. Patients are either selected by their appointments or by searching and selecting their name. The complete content is stored on the local computer from which the utility was executed. The extracted data is password protected and fully encrypted in case the PC’s security is compromised.
What can TCMS-to-Go be used for?
The purpose of the TCMS2Go utility is to have local data viewing access in case of connectivity loss, with an internet based system or if an office based server were to fail. It must be run prior to any system failure. You cannot add to the system when viewing. Walk-in patients will not appear as it is based on scheduled patients only. It can also be used if a provider wished to extract their data for later reference, isolated from the original system.
The extraction utility is currently based on an appointment period only. Either select future period, to guard against connectivity loss or select the historic date span for the installed system for a complete patient population extraction.
Other important notes about TCMS-to-Go
• The process is for viewing data only.
• The longer the query period the longer it will take to run and extract the data.
• The PC will be inoperable for other activity during the extraction process.
• We cannot construct file data from any extracts as this program is for viewing patient data in a secure setting.
• There is no ability to create file data from this extraction.
New options available while exporting TCMS-to-Go
There are new options available in the TCMS-to-Go module while exporting the data, including cutoff dates for documents (base on creation date), and the option to export patient’s insurance cards if they are scanned in.
 |
| Click Image to Enlarge |
TCMS-to-Go exports can now include multiple resources.
 |
| Click Image to Enlarge |
TCMS-to-Go now allows user to search by account or patient’s last name
 |
| Click Image to Enlarge |
A Claim Center’s name was modified
The name of the Claim Center for DME Travelers has been modified to DME MAC to accommodate some recent changes made by the clearinghouse.
 |
| Click Image to Enlarge |
The label for “Scanned Images” in Documents Setup was modified
For clearer understanding, the document type in the Documents Setup section named “Scanned Images” has been modified to read, “TIF – Scanned or Faxed”.
 |
| Click Image to Enlarge |
There are now alternative fields available for “Billing” and “Pay to” addresses
TCMS now offers additional fields in the Provider Number Setup screen that allow for alternative Billing and Pay-to addresses when submitting claims electronically. These fields are available specifically for use with any carrier/payer, provider and location combination. Address-related data in these fields will replace any existing Billing or Pay-to convention.
There is no change or action necessary to continue to bill the way you already are… these fields will serve as alternatives to what you may already be using. Selection of a Practice Default is necessary to activate this new feature.
 |
| Click Image to Enlarge |
Below is a schematic of the scripted building of Billing Address and of the Pay-to Address logic in TCMS. Please call us if you have any questions regarding these additions.
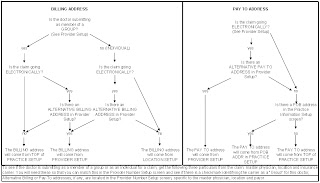 |
| Click Image to Enlarge |
Bulk Eligibility is now fully functional in 5010 for CheckMedicare and Emdeon
Eligibility check for secondary and tertiary carriers is now available
There is a Practice Default that, when selected, will check a patient’s Secondary and Tertiary Insurances if they exist.
 |
| Click Image to Enlarge |
New Custom Field available for patients with End-Stage Renal Disease
There is a new Patient Custom Field. “Medicare Secondary End-Stage Renal Disease”. Setting this to “Yes” from the Patient’s Demographic screen will result in the building of a value of “13” in loop 2000B SBR.
 |
| Click Image to Enlarge |
Friday, April 13, 2012
TCMS Version 4.7.8 – What’s New, What’s Fixed, etc
A new option that prevents changing a charge amount while updating
Some background:
Prior to this version, when a service line is updated to a different carrier, and the fee schedule for the new carrier has a different charge amount in its fee schedule, the original charge amount changes to the new charge amount, unless:
(1) A payment was previously posted to the service
(2) A write-off was previously applied to the service
(3) The service was performed in a closed month
About this new option:
There is now a new option that the user can select while updating claims: “Do not update charge amount”.
If this new option is selected, and there is a difference between the charge amounts of the two fee schedules utilized, the charge amount of the service will not change when the service is updated to the new insurance profile.
Using the "Repeat Charge" feature with a future service date is now prevented
The "Repeat Charge" feature saves time when the same service needs to be re-written. But writing a service with a future DOS is not usually a desired option, and the “Repeat Charge” feature was inadvertently permitting this if the batch date was set with a date in the future. This is now no longer possible… if the user attempts to write a future service while using the future batch bate option, a message will be generated notifying the user that a future date of service cannot be used.
ERN Kicklist now includes Claim Adjustment codes
The ERN Kicklist report is an on-screen display that identifies the payments that were unable to be posted while posting payments automatically from an ERN/ERA. This report will now include the Claim Adjustment codes which can be used to sort/order the results of the report.
Unsent No Fault/Worker’s Comp Claims now included in report
The No Fault and Worker’s Compensation Claims now follow the same rules as all other claims when the Unsent Claims report is generated. Claims that have not yet been sent electronically (WC Claims can now be submitted electronically through iHCFA) or printed will appear on the Unsent Claims report.
Eligibility is now available for CheckMedicare as well as Emdeon
The Eligibility feature in TCMS offers eligibility and benefits verification with the largest group of commercial and government payers in the industry through which accurate eligibility information can be verified in real-time or high-volume batches. This feature, while working well using Emdeon, was recently not working with CheckMedicare and is now available .
ASP/Cloud clients can now select a preferred SS# default
There is a Practice Default that was already available to all clients, except for ASP/Cloud clients. The default is specific to retaining patient social security numbers in the patient demographics screens. This default is now also available to ASP clients.
Some background:
Prior to this version, when a service line is updated to a different carrier, and the fee schedule for the new carrier has a different charge amount in its fee schedule, the original charge amount changes to the new charge amount, unless:
(1) A payment was previously posted to the service
(2) A write-off was previously applied to the service
(3) The service was performed in a closed month
About this new option:
There is now a new option that the user can select while updating claims: “Do not update charge amount”.
If this new option is selected, and there is a difference between the charge amounts of the two fee schedules utilized, the charge amount of the service will not change when the service is updated to the new insurance profile.
Using the "Repeat Charge" feature with a future service date is now prevented
The "Repeat Charge" feature saves time when the same service needs to be re-written. But writing a service with a future DOS is not usually a desired option, and the “Repeat Charge” feature was inadvertently permitting this if the batch date was set with a date in the future. This is now no longer possible… if the user attempts to write a future service while using the future batch bate option, a message will be generated notifying the user that a future date of service cannot be used.
ERN Kicklist now includes Claim Adjustment codes
The ERN Kicklist report is an on-screen display that identifies the payments that were unable to be posted while posting payments automatically from an ERN/ERA. This report will now include the Claim Adjustment codes which can be used to sort/order the results of the report.
Unsent No Fault/Worker’s Comp Claims now included in report
The No Fault and Worker’s Compensation Claims now follow the same rules as all other claims when the Unsent Claims report is generated. Claims that have not yet been sent electronically (WC Claims can now be submitted electronically through iHCFA) or printed will appear on the Unsent Claims report.
Eligibility is now available for CheckMedicare as well as Emdeon
The Eligibility feature in TCMS offers eligibility and benefits verification with the largest group of commercial and government payers in the industry through which accurate eligibility information can be verified in real-time or high-volume batches. This feature, while working well using Emdeon, was recently not working with CheckMedicare and is now available .
ASP/Cloud clients can now select a preferred SS# default
There is a Practice Default that was already available to all clients, except for ASP/Cloud clients. The default is specific to retaining patient social security numbers in the patient demographics screens. This default is now also available to ASP clients.
Friday, March 16, 2012
TCMS Version 4.7.7 – What’s New, What’s Fixed, etc
The Collections Module has a handful of new enhancements and modifications:
In the Setup screen for the Collection Module, there are now new options to further define the criteria for moving Insurance-Due claims into Collections. The user is now able to set the minimum number of aging days based on service date in addition to transaction date.
On the “Move Claims” screen, the user will now be given the option to move claims by calculating the aging date from the service date or from the transaction date as in previous versions of TCMS.
Additionally, the Agent work screen will now display each individual claim assigned to the selected agent rather than displaying the information on an account level. This allows the agent to work their assigned claims directly from this screen and eliminates the need to switch between screens. The detail grid will now also include the “Transaction Aging Days”, “Service Aging Days”, and “Date Assigned” columns to allow the user further flexibility to sort claims as desired.
For Assigned and Worked claims, in addition to the existing ledger display at the bottom of the screen, new tabs have been added to give the user access to the Patient’s Demographic and Insurance information without having to switch screens or exit the Collection module.
If the user ‘Right Mouse’ clicks and selects to jump to the patient’s Ledger from the Agent work screen, it will bring the user to the actual claim. This is a big time saver as the user will not have to search through claims.
We have also added the “Agent Productivity Report” under the Collection reports menu.
This Report can be run for selected agents in a selected date span.
The Report can be run in Summary mode:
Or in Detail Mode:
Electronic Worker’s Comp is now updated with new iHCFA requirements
Electronic Worker’s Comp claim submissions, processed through the WCB certified clearinghouse iHCFA, are now updated to the latest compliance requirements.
No Fault claim form data adjustment
The No Fault claim form was only including the first claim modifier and cutting off any other existing modifier codes. The form will no longer cut off secondary modifiers when printed.
Workplace Health Statements now observe Practice PO Box addresses
The Workplace Health Statements will now utilize the Practice’s PO Box Pay-to address (if used for the practice in the Practice Setup screen).
Facilities can now be removed from claims by the user
In prior versions, the user was always able to change a claim’s facility from one to another; but there was a limitation on completely removing a facility altogether. The user can now remove a facility without the need to replace it with another.
The EMC Submissions report has 2 new indicators
The EMC Submissions report will now indicate if a claim has exceeded the Timely Filing Warning level assigned in the Insurance Carrier’s Setup screen; the report will also now indicate if a claim has exceeded the Timely Filing Allowance level, also assigned in the carrier’s setup screen.
A new option to claim acknowledgements
Until now, the user was unable to view the Medicaid 277 report, which offers information on claims that were rejected. There is a menu option available under the ‘Claims’ menu called ‘View Claim Acknowledgement’. Once launched, the user can select from downloaded 999 or 277CA files to view, save, or print.
In the Setup screen for the Collection Module, there are now new options to further define the criteria for moving Insurance-Due claims into Collections. The user is now able to set the minimum number of aging days based on service date in addition to transaction date.
 |
| Click Image to Enlarge |
 |
| Click Image to Enlarge |
 |
| Click Image to Enlarge |
 |
| Click Image to Enlarge |
 |
| Click Image to Enlarge |
 |
| Click Image to Enlarge |
 |
| Click Image to Enlarge |
The Report can be run in Summary mode:
 |
| Click Image to Enlarge |
Or in Detail Mode:
 |
| Click Image to Enlarge |
Electronic Worker’s Comp is now updated with new iHCFA requirements
Electronic Worker’s Comp claim submissions, processed through the WCB certified clearinghouse iHCFA, are now updated to the latest compliance requirements.
No Fault claim form data adjustment
The No Fault claim form was only including the first claim modifier and cutting off any other existing modifier codes. The form will no longer cut off secondary modifiers when printed.
Workplace Health Statements now observe Practice PO Box addresses
The Workplace Health Statements will now utilize the Practice’s PO Box Pay-to address (if used for the practice in the Practice Setup screen).
Facilities can now be removed from claims by the user
In prior versions, the user was always able to change a claim’s facility from one to another; but there was a limitation on completely removing a facility altogether. The user can now remove a facility without the need to replace it with another.
The EMC Submissions report has 2 new indicators
The EMC Submissions report will now indicate if a claim has exceeded the Timely Filing Warning level assigned in the Insurance Carrier’s Setup screen; the report will also now indicate if a claim has exceeded the Timely Filing Allowance level, also assigned in the carrier’s setup screen.
A new option to claim acknowledgements
Until now, the user was unable to view the Medicaid 277 report, which offers information on claims that were rejected. There is a menu option available under the ‘Claims’ menu called ‘View Claim Acknowledgement’. Once launched, the user can select from downloaded 999 or 277CA files to view, save, or print.
Wednesday, March 7, 2012
TCMS Version 4.7.6 – What’s New, What’s Fixed, etc
Introducing the new “Copay Analysis” Report
There is a new report under the “Scheduler Reports” section of TCMS, it is a Copay Analysis Report. The report compares “Copay” payments applied to the accounts of patients that were scheduled (within a specific date or date span) to their expected copay amount in the same patient’s Demographics screen. The report will then identify exact payment matches and payment exceptions (whether the patient paid more or less than the expected amount). The user can opt to only show exceptions, or limit by Resources, and an assortment of other options… including generating a report for a specific patient by account number.
The Unit Analysis Report is now a bit faster
The Unit Analysis report is now faster and offers better response times to accommodate all levels of Oracle databases.
Worker’s Comp Authorizations will all display
When selecting the “Show All” authorizations option in the Worker’s Comp Claim Edit screen, all available authorizations will now display (regardless of which insurance carrier generated the authorization). This is because, unlike medical claim authorizations, WC authorizations are often carried over to other payors and need to be selectable for any claims.
Zero payments will now post from ERN’s
When posting from an ERN, zero-dollar payments will now post to the patient’ claim as long as there is either a copay or deductible applied to the service.
There is a new report under the “Scheduler Reports” section of TCMS, it is a Copay Analysis Report. The report compares “Copay” payments applied to the accounts of patients that were scheduled (within a specific date or date span) to their expected copay amount in the same patient’s Demographics screen. The report will then identify exact payment matches and payment exceptions (whether the patient paid more or less than the expected amount). The user can opt to only show exceptions, or limit by Resources, and an assortment of other options… including generating a report for a specific patient by account number.
The Unit Analysis Report is now a bit faster
The Unit Analysis report is now faster and offers better response times to accommodate all levels of Oracle databases.
Worker’s Comp Authorizations will all display
When selecting the “Show All” authorizations option in the Worker’s Comp Claim Edit screen, all available authorizations will now display (regardless of which insurance carrier generated the authorization). This is because, unlike medical claim authorizations, WC authorizations are often carried over to other payors and need to be selectable for any claims.
Zero payments will now post from ERN’s
When posting from an ERN, zero-dollar payments will now post to the patient’ claim as long as there is either a copay or deductible applied to the service.
TCMS Version 4.7.4 – What’s New, What’s Fixed, etc
A new Practice Default available for Faxes
Until now, a document could only be faxed if it were digitally signed. We’ve added a new Practice Default that, when it is UNCHECKED, will allow users to fax documents that are not digitally signed.
Claim files removed properly after sending
When electronic claim files (EMC files) are generated for submissions to Emdeon or to McKesson, they are temporarily held in a file and are usually removed after the submission was completed. Recently, however, the files were not disappearing… this problem is now addressed. The EMC files in the folder will now be removed from the folder after they are submitted to the clearinghouse for both Emdeon and McKesson.
New Worker’s Comp form now available
For Workers Compensation, there is a new version of the C 4.3 form. It is identified by (1/12) at the bottom of the form.
* The Worker’s Compensation forms will now adhere to the Pay-To address if it is selected in the Practice Setup screen.
Appointment history will now print
Printing a patient’s appointment history was causing an error when the option to “Show cancelled appointments” was selected. This has now been addressed.
New 64-bit station Installer available
There is a new Installer for users that are utilizing 64-bit workstations that need to send and/or process claims electronically. The new Installer is available in the folder where the TCMS runtimes are located. It is called the “CriterionsEDIDownloaderx64Setup.msi”
Until now, a document could only be faxed if it were digitally signed. We’ve added a new Practice Default that, when it is UNCHECKED, will allow users to fax documents that are not digitally signed.
Claim files removed properly after sending
When electronic claim files (EMC files) are generated for submissions to Emdeon or to McKesson, they are temporarily held in a file and are usually removed after the submission was completed. Recently, however, the files were not disappearing… this problem is now addressed. The EMC files in the folder will now be removed from the folder after they are submitted to the clearinghouse for both Emdeon and McKesson.
New Worker’s Comp form now available
For Workers Compensation, there is a new version of the C 4.3 form. It is identified by (1/12) at the bottom of the form.
* The Worker’s Compensation forms will now adhere to the Pay-To address if it is selected in the Practice Setup screen.
Appointment history will now print
Printing a patient’s appointment history was causing an error when the option to “Show cancelled appointments” was selected. This has now been addressed.
New 64-bit station Installer available
There is a new Installer for users that are utilizing 64-bit workstations that need to send and/or process claims electronically. The new Installer is available in the folder where the TCMS runtimes are located. It is called the “CriterionsEDIDownloaderx64Setup.msi”
Friday, January 6, 2012
TCMS version 4.7.3 - What’s New, What’s Fixed, etc.
TEMPORARILY SUSPEND SENDING BCBS CLAIMS
MedXpress and BCBS were experiencing transmission irregularities for 4010 & 5010 Formats. We all understand the urgency… expect a correction shortly. We can notify all clients instantly through this messaging once this is addressed. Please do not call Criterions support for BCBS claims until there is notification that it has been corrected or we have provided instructions with this type of “Alert”. We will notify all clients when and how to resume BCBS submissions once we get notice from them.
MEDICARE HAS EXTENDED THE 4010 FORMAT THROUGH JAN 31
Although many clients are submitting 5010 Medicare formats without issue we have discovered irregularities related to Windows workstation configuration variables. If you experience 5010 submission errors, you can revert to the 4010 format as a temporary solution as we are working with those clients for a remedy. The selection is found under “File”, “Setup”, “Practice Setup”, “Practice Defaults” and remove the checkmark on the default labeled “Generate 5010 Claims” – this will permit you to generate a file in the older 4010 format.
The 5010 version has been re-released. Version 4.7.3 addresses the following irregularities discovered with the earlier release: Only update if this affects you.
CMS-1500 (HCFA) forms will now generate PO Box info if applicable
Box 33 on the CMS 1500 (HCFA) was not printing the PO BOX PAY TO address when the new PO Box feature became available and selected for the Practice (TCMS was printing the Practice Address). This issue is now addressed. When the PO Box feature in the TCMS Practice Information screen is utilized, TCMS will now print the PO Box “Pay To” address information in Box 33 of the HCFA.
Patient Statements will now generate PO Box info if applicable
Patient Statements were not printing the PO BOX PAY TO address when the new PO Box feature became available and selected for the Practice (TCMS was printing the Practice Address). This issue is now addressed. When the PO Box feature in the TCMS Practice Information screen is utilized, TCMS will now print the PO Box “Pay To” address information under the Practice Name on printed patient statements (both bulk printing and individual printing). This issue is also addressed when Electronic statement files are generated.
Creating an electronic file for individual/selected carriers
Creating a claim file for “Individual Insurance Carriers” was not excluding unselected carriers. This issue is now addressed… only the claims due from selected carriers will be included
Procedure Code Financial Analysis Report sort correction
The Procedure Code Financial Analysis Report was not printing in the correct sort order when a specific combination of selections was selected (include patient name and split by Insurance type/Carrier). The resulting sort order for this specific report was incorrect. This issue is now addressed.
Worker’s Comp “MG-2” form misspelling corrected
There was a misspelling on the MG-2 form that is now corrected.
MedXpress and BCBS were experiencing transmission irregularities for 4010 & 5010 Formats. We all understand the urgency… expect a correction shortly. We can notify all clients instantly through this messaging once this is addressed. Please do not call Criterions support for BCBS claims until there is notification that it has been corrected or we have provided instructions with this type of “Alert”. We will notify all clients when and how to resume BCBS submissions once we get notice from them.
MEDICARE HAS EXTENDED THE 4010 FORMAT THROUGH JAN 31
Although many clients are submitting 5010 Medicare formats without issue we have discovered irregularities related to Windows workstation configuration variables. If you experience 5010 submission errors, you can revert to the 4010 format as a temporary solution as we are working with those clients for a remedy. The selection is found under “File”, “Setup”, “Practice Setup”, “Practice Defaults” and remove the checkmark on the default labeled “Generate 5010 Claims” – this will permit you to generate a file in the older 4010 format.
The 5010 version has been re-released. Version 4.7.3 addresses the following irregularities discovered with the earlier release: Only update if this affects you.
CMS-1500 (HCFA) forms will now generate PO Box info if applicable
Box 33 on the CMS 1500 (HCFA) was not printing the PO BOX PAY TO address when the new PO Box feature became available and selected for the Practice (TCMS was printing the Practice Address). This issue is now addressed. When the PO Box feature in the TCMS Practice Information screen is utilized, TCMS will now print the PO Box “Pay To” address information in Box 33 of the HCFA.
Patient Statements will now generate PO Box info if applicable
Patient Statements were not printing the PO BOX PAY TO address when the new PO Box feature became available and selected for the Practice (TCMS was printing the Practice Address). This issue is now addressed. When the PO Box feature in the TCMS Practice Information screen is utilized, TCMS will now print the PO Box “Pay To” address information under the Practice Name on printed patient statements (both bulk printing and individual printing). This issue is also addressed when Electronic statement files are generated.
Creating an electronic file for individual/selected carriers
Creating a claim file for “Individual Insurance Carriers” was not excluding unselected carriers. This issue is now addressed… only the claims due from selected carriers will be included
Procedure Code Financial Analysis Report sort correction
The Procedure Code Financial Analysis Report was not printing in the correct sort order when a specific combination of selections was selected (include patient name and split by Insurance type/Carrier). The resulting sort order for this specific report was incorrect. This issue is now addressed.
Worker’s Comp “MG-2” form misspelling corrected
There was a misspelling on the MG-2 form that is now corrected.
Subscribe to:
Posts (Atom)













